Subtitle
Treating Hodgkin and non-Hodgkin lymphoma with proton therapy
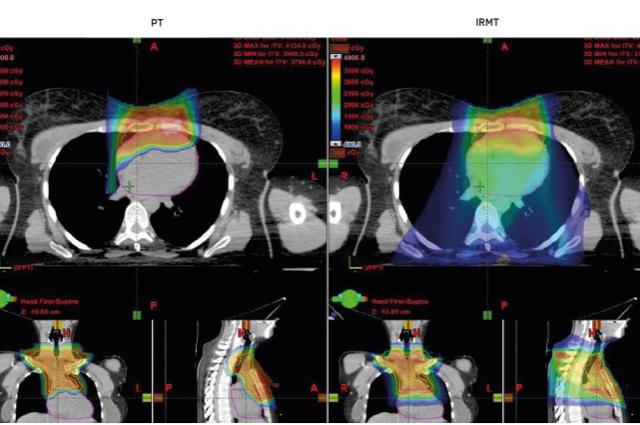
Proton therapy is different from photon-based radiotherapy. Because of their unique physical properties, protons have no ‘exit’ dose and very little ‘entrance’ dose. Proton therapy is able to achieve statistically significant and clinically relevant dose reduction, as numerous in silico studies have demonstrated. In addition to overall integral dose reduction, proton plans lend themselves best to achieving organ specific dose reduction for heart, lung, esophagus, breast and other structures. A comparison study on estimated risks of cardiovascular disease and secondary lung and breast cancers attributable to 3DCRT, volumetric modulated arc therapy (VMAT) and proton therapy shows proton therapy as the superior modality that results in the least life years lost.
The latest development of proton delivery technique – pencil beam scanning (PBS) – enables further reduction of mean lung dose, mean heart dose and internal target volume. The number of clinical outcome studies is increasing, particularly prospective studies. Reported data has shown encouraging disease control and an expected reduction in long-term adverse effects, given the minimized target volume and significant dose reduction to normal tissue. Lymphoma patients treated with proton followed for longer term data.

